 Practical Practitioner
Practical Practitioner
By: Pamela Egan, DNP, CDE
National Menopause Month: When is Hormone Replacement Therapy Appropriate?
Has your quality of life come to a dead stop? Suddenly, you can’t sleep at night, gained weight, became fuzzy minded, anxious and depressed, have no interest in sex, yet when you ask to have your hormones checked you are told that hormone replacement therapy is bad for you and will cause heart attacks, strokes, and breast cancer. So what’s a woman to do?
With the advent of Anti-Aging & Regenerative Medicine, we actually have a large group (30,000) physicians and health care providers across the world reviewing the research and looking exactly at what happens to our bodies when they become depleted of hormones and nutrients. Take a 38 year old woman who has had a complete hysterectomy. Hormonally, she is equal to a 50 year old woman. How do you want to live these years? Our disease based medical system is merely the treatment of existing disease. She may receive prescriptions for Prozac, Xanax, and Ambien but is still left with the underlying imbalances that caused the depression, anxiety, and insomnia in the first place. Given the choice; would you not choose to restore optimal function and prevent these miserable symptoms all together?
Restoring balance means optimizing the ability of our cells to do what they do best: keep us healthy, happy, energetic, prevent cancer, heart disease, and other chronic diseases. This involves correcting deficiencies of hormones, nutrients, removing toxins, maintaining active, strong bodies, and being at peace with oneself.
We age because our hormones decline, not the other way around. In women and men, hormone imbalances occur from age 30 onwards. By age 50, we are at approximately 50% of hormone function for estrogen, progesterone, testosterone, thyroid, DHEA, melatonin and growth hormone. Of course, a healthy lifestyle, diet, genes play an important role in optimizing cellular function; however, at some point our organs will not produce hormones even with the healthiest lifestyle and the best genes.
Symptoms are one reason that people restore hormones; but the more compelling reason is the potential to prevent degenerative disease, since symptoms can be handled by a variety of other ways. Studies show that every brain cell in the body has a receptor for thyroid, estrogen, progesterone and testosterone, as does every heart cell, every nerve cell, every bone cell, every vascular cell and every skin cell. It becomes clear that as hormone levels decline, the cells degenerate leading to a myriad of symptoms such as sexual decline, fatigue, anxiety, mood swings, weight gain, insomnia, cognitive decline, but more importantly degenerative disease.
In women, the first hormone to decline is progesterone around age 35. This produces symptoms such as anxiety, insomnia, PMS, mood swings, fibroids, breast and ovarian cysts, heavy or irregular bleeding and weight gain. Progesterone also builds bone.
In women, estrogen levels begin to decline and become imbalanced around age 45 and eventually wane altogether at age 51, the time of official menopause. Changing estrogen levels produce hot flashes, skin and vaginal dryness, recurrent urinary infections, urinary incontinence, bone loss and cognitive decline.
Testosterone declines in men and women from the late 30’s onward producing loss of desire for sex, joint and bone pain, muscle weakness, loss of confidence, moodiness, depression, anxiety, muscle loss and fat gain. Studies show that testosterone repletion supports a protective role for testosterone against heart disease, cognitive decline and bone loss.
Other hormones include thyroid, insulin, DHEA, Melatonin, Pregnenolone, Growth Hormone.
When women consider hormone replacement therapy, the alarming question is about the risk, especially breast cancer, strokes and heart attacks. Why do you think women are most protected in their 20’s & 30’s when they have the highest hormone levels? It is only after menopause that women have increased risk of stroke, heart attack and breast cancer. We know that most breast cancers occur after menopause; precisely at the time when the ovaries stop producing the normal balance of hormones.
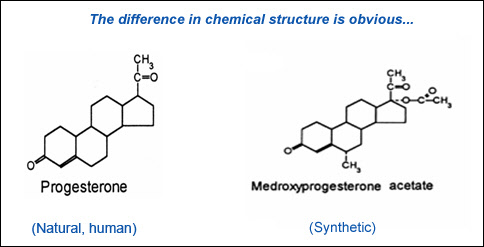
Large studies like the Women’s Health Initiative (WHI) used synthetic hormones or chemicals (not identical to human hormones) with a ratio of estrogen weighted towards the bad estrogen estrone (E1), whereas estradiol (E2) and estriol (E3) have protective effects on the body. Progestins (as used in WHI) have been shown to increase clots and breast cancer in 5 trials compared with natural “progesterone” which is associated with protection. Bio-identical Estradiol (E2) delivered through the skin decreases clots and therefore the risk of cardiac and vascular events in the brain, as opposed to estrone (E1) delivered through the mouth (oral Premarin used in WHI).
So, when restoring hormones, use protective forms and delivery routes. Use only the forms of hormones, which are exactly identical to the body’s molecular structure (bio-identical hormones). These can be compounded in a Compound Pharmacy or we now have prescriptions that are bio-identical such as Prometrium(Progesterone) and Climara or Vivelle Dot (Estradiol). Estriol, which prevents collagen loss and breast cancer, must be obtained from a Compound Pharmacy.
Hormone replacement should always be accompanied by the nutrients that activate the hormone receptor and removal of toxins that may interfere with the activity of the nutrients or hormones.
Hormone function is more important than a hormone level. So, even though your thyroid hormone may measure normal, you may not have optimal thyroid function.
To achieve optimal function of hormones it is necessary to use a little bit of each deficient hormone, since they activate each other, instead of a whopping dose of one like DHEA, with hopes that it converts to the others.
There is no magic pill to balance Cortisol and high insulin. Therefore, these hormones require attention to stress reduction, adrenal support, detoxification, lifestyle changes and insulin support.
Preservation depends on restoration of hormone levels.
Dr. Pamela Egan: Adult & Family Nurse Practitioner
Doctor of Nursing Practice
MS, Metabolic & Nutritional Medicine
Fellow, Metabolic Medical Institute
MN, Gerontology Mental Health
Certified Diabetes Educator
She can be reached at 985-892-3031 or www.pamelaegan.com.
Recent Posts:
- – Vitamin D3 is far superior to Vitamin D2
- – Natural Remedies for Colds and Upper Respiratory Infections
- – What is Swine Flu and What are its Symptoms?
- – Andropause: Male Menopause Caused By Testosterone Deficiency
- – Anti-Aging Medicine: Myth Or Reality?
PamelaEgan.com > Health Articles > Women’s Health

